Psoriasis is a chronic skin condition, but it is not the only disorder that can produce red, scaly patches on the skin. Several other conditions closely resemble psoriasis in appearance, which can make self-identification difficult. Understanding how these conditions differ is essential for effective treatment. In this guide, we explore conditions that mimic psoriasis, highlight key distinctions, and provide practical insights to support informed discussions with a healthcare professional.
Understanding Psoriasis
Before comparing similar conditions, it helps to establish what defines psoriasis itself. Psoriasis is an autoimmune disorder that causes red, scaly patches of skin. These patches most commonly appear on the lower back, elbows, knees, and scalp. The condition develops when skin cells build up too quickly, leading to visible inflammation and discoloration. While the exact cause is not fully understood, genetic factors and immune system dysfunction are widely believed to play significant roles in its development.
Common Conditions Mistaken for Psoriasis
Because psoriasis shares visible traits with several other skin disorders, confusion is common. Distinguishing psoriasis from similar conditions is important to ensure proper diagnosis and appropriate treatment. When a condition is misidentified, management may be ineffective, leading to prolonged discomfort. For this reason, a correct diagnosis is often the first step toward controlling symptoms and improving overall quality of life.
Eczema
One of the most frequently confused conditions is eczema, also known as atopic dermatitis. Eczema shares similarities with psoriasis, such as red and inflamed skin. However, eczema typically causes intense itching, swelling, and oozing of clear fluid, which are less common in psoriasis. The itching associated with eczema can be particularly severe and often leads to repeated scratching, worsening inflammation over time.

In terms of location, eczema tends to occur in skin folds, such as behind the knees or elbows, as well as on the hands, feet, and face. Psoriasis, by contrast, more often appears on the outer surfaces of joints, which can help differentiate the two.
Seborrheic Dermatitis
Another condition commonly mistaken for psoriasis is seborrheic dermatitis. This disorder primarily affects areas rich in oil glands, including the scalp, face, and upper chest. Like psoriasis, it can cause redness, scaling, and irritation.
Despite these similarities, seborrheic dermatitis scales are usually greasy, flaky, and yellowish, while psoriasis scales tend to be thicker, well-defined, and white or silvery. When the scalp is involved, distinguishing between the two can be challenging, but the oily texture of seborrheic dermatitis scales often provides an important clue.
Tinea Corporis
Tinea corporis, commonly known as ringworm, differs from psoriasis in both cause and presentation. Unlike psoriasis, tinea corporis is a fungal infection rather than an autoimmune condition. It typically appears as a ring-shaped rash with a clearer center and a raised, scaly border.
In addition to its distinctive shape, tinea corporis is often itchy and can spread through direct contact with an infected person or animal. Diagnosis is usually straightforward and can be confirmed through a simple skin scraping examined under a microscope, revealing fungal elements.
Lichen Planus
Lichen planus is another inflammatory condition that may resemble psoriasis at first glance. It presents as shiny, flat-topped, purple or reddish-purple bumps that are often itchy. These lesions most commonly appear on the wrists, ankles, or inside the mouth and may display fine white lines on their surface, known as Wickham's striae.
Psoriasis, in comparison, typically produces thicker, scaly patches that are red or pink rather than purple. Nail changes, such as pitting or discoloration, are also more commonly associated with psoriasis, although both conditions can occasionally affect the nails.
Pityriasis Rosea
Pityriasis rosea has a presentation that can initially be confused with psoriasis, particularly in early stages. This condition often begins with a single, large, oval “herald” patch on the chest, abdomen, or back. Over time, smaller oval lesions spread outward in a distinctive tree-like or “Christmas tree” pattern.
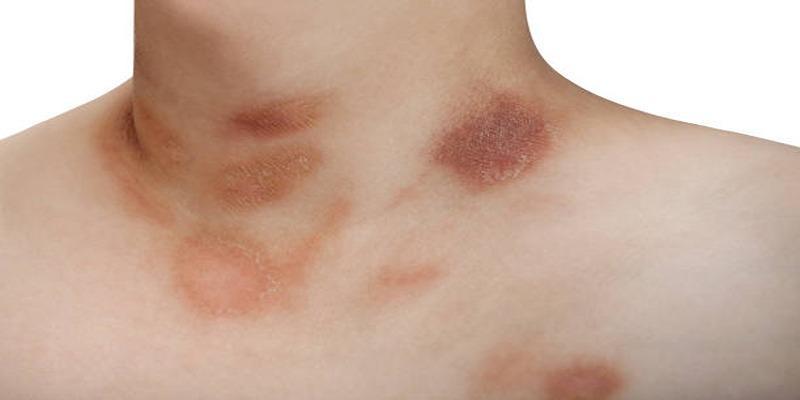
This distribution pattern is a key distinguishing feature. Pityriasis rosea is usually temporary, lasting about six to eight weeks before resolving on its own. This contrasts with psoriasis, which is chronic and persistent. While the rash may be mildly itchy, its predictable progression helps differentiate it from psoriasis plaques.
Diagnosing Psoriasis vs. Similar Conditions
When evaluating persistent or unexplained skin changes, careful distinction between psoriasis and similar conditions is essential. Although many of these disorders share overlapping features, each presents unique characteristics that guide diagnosis. Recognizing these differences allows healthcare providers to select appropriate treatments and avoid unnecessary interventions.
Unique Features of Psoriasis
Psoriasis is characterized by well-defined, raised plaques covered with silvery-white scales, most often appearing on the scalp, elbows, and knees. In some cases, the plaques may bleed when scratched, a feature known as the Auspitz sign. Beyond skin symptoms, psoriasis can also involve systemic effects, including joint pain associated with psoriatic arthritis, which is not typical of many look-alike conditions.
Treatment and Management Approaches
Although these conditions may appear similar, treatment and management strategies vary significantly. Accurate diagnosis is therefore critical, as effective care depends on addressing the underlying cause rather than just surface symptoms. Managing psoriasis often requires a long-term, individualized approach.
Treatment Options for Psoriasis
Psoriasis treatment commonly involves a combination of therapies. These may include topical medications such as corticosteroids or vitamin D analogs, as well as phototherapy or systemic treatments for more severe cases. In addition to medical treatment, lifestyle adjustments like stress management and maintaining a healthy weight can play an important role in reducing flare-ups and supporting long-term control.
General Skincare Recommendations
Regardless of diagnosis, good skincare practices support skin health and symptom relief. Using gentle, fragrance-free cleansers and applying moisturizers regularly can help reduce irritation and promote healing. Sunscreen protects affected skin from UV damage, while avoiding scratching lowers the risk of secondary infections and further inflammation.
When to Consult a Specialist?
Professional dermatological care should be considered when symptoms are severe, persistent, or worsening. Signs of infection, such as increased redness, oozing, or fever, also warrant medical attention. If over-the-counter treatments fail or symptoms begin to interfere with daily activities, consulting a specialist is recommended.
Before an appointment, noting symptom patterns, potential triggers, and previously tried treatments can help the dermatologist assess the condition more effectively and develop a tailored care plan.
Conclusion
Psoriasis shares visible features with several other skin conditions, which can make accurate identification challenging. Understanding the key differences between these disorders helps guide proper care and symptom management. When skin changes persist or affect daily life, seeking evaluation from a qualified specialist supports timely diagnosis, appropriate treatment, and improved long-term skin health.